Arizona RESTEP –
NIH T32 pre-doctoral training program
Training the next generation of innovators in regenerative medicine
What is RESTEP?
Arizona’s Regenerative Engineering, Science and Technology Education, or RESTEP, is an NIH T32 pre-doctoral training program designed to develop trainees into change makers ready to develop and translate regenerative medicine technologies into the clinic and bioindustry (T32GM154654).
If you’re passionate about regenerative medicine and translational science, RESTEP gives you the tools, skill sets, experiences and connections to turn research discoveries into innovations that improve human health.
What can I expect as a RESTEP trainee?
RESTEP will prepare eight doctoral students per year to become well-rounded leaders in regenerative medicine, a field that focuses on repairing or replacing damaged or diseased tissues and organs.
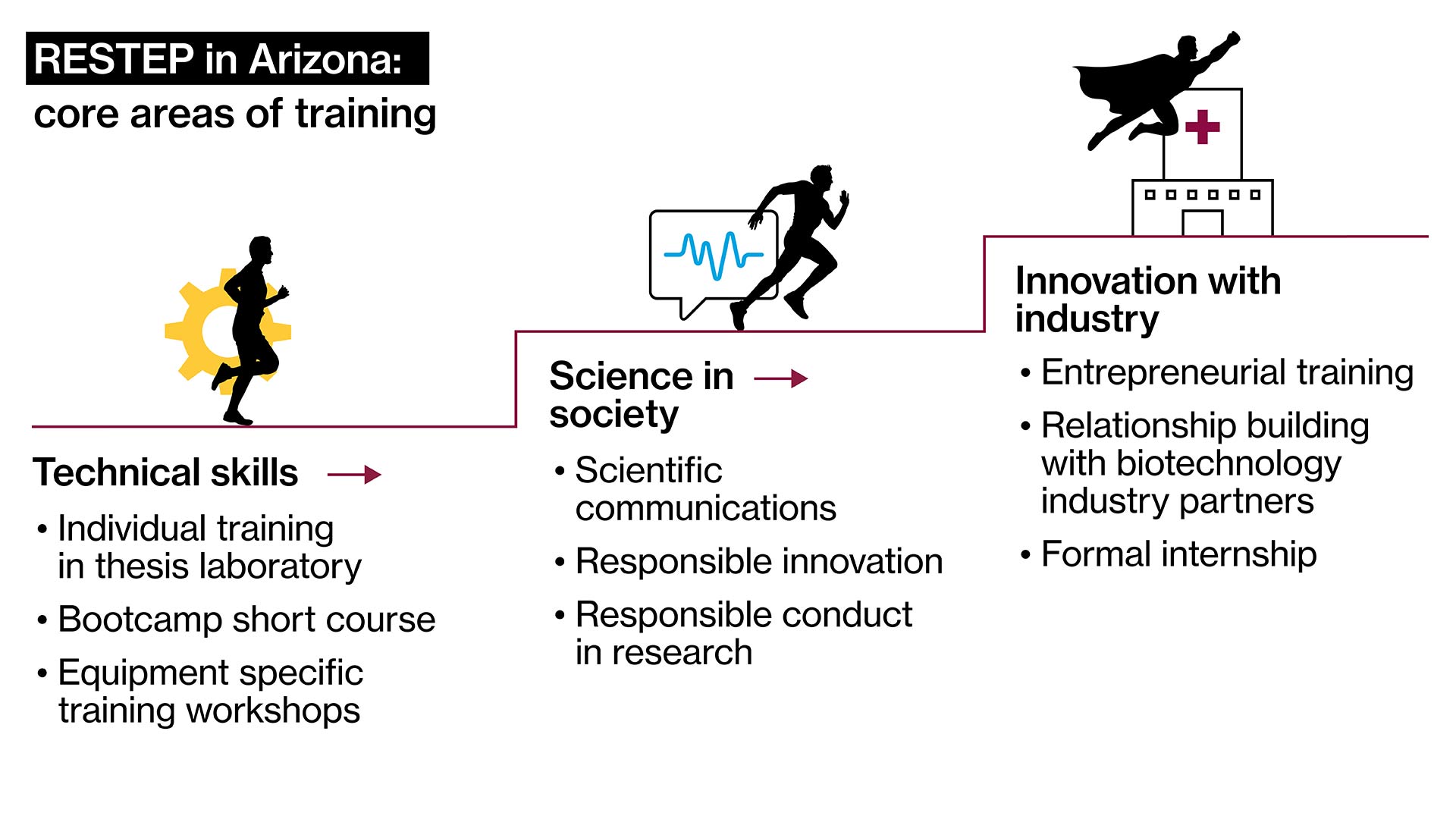
The two-year curriculum emphasizes the importance of connecting science to society and taking knowledge beyond the lab. RESTEP will provide experiences to support success in multiple career areas, including:
- Research and training in your thesis lab.
- Hands-on experience working in laboratories of the Regenerative Medicine Core, in advanced areas such as stem cell biology, tissue engineering, biomaterials development and gene and cell therapies.
- Knowledge of entrepreneurship practices, intellectual property and the process of responsively translating laboratory discoveries into therapies and technologies.
- Internships and workshops on commercialization and ample opportunities to build professional networks with local industry leaders.
How is RESTEP funded?
RESTEP is funded by The National Institute of General Medical Sciences, or NIGMS, and supports trainees from these four PhD programs:
What is included in RESTEP support?
- Stipend
- Tuition
- Health insurance
- Travel
- Childcare costs
Apply in May at the end of your first PhD year. Funding is awarded for up to two years.
RESTEP student trainees
My research is developing cell-based therapies for autoimmune Type 1 Diabetes by integrating complex hydrogel geometries for islet encapsulation by enhancing oxygen transport and preventing direct antigen recognition and trophoblast-derived immunomodulatory cells to suppress indirect immune response against the implanted islets for improved insulin secretion.
Hi, my name is Maksym Dankovskyy, and I’m a PhD student in Dr. Robin Harris’s lab. My project focuses on understanding how damage responsive enhancers are silenced with development in Drosophila melanogaster. These enhancers are regions of DNA that drive the expression of crucial, pro-regenerative genes at sites of injury.
Polytrauma-traumatic brain injury (PT-TBI) is when a patient sustains a traumatic brain injury with significant secondary trauma injuries. PT-TBI can cause platelet deficiencies, persistent neuroinflammation, and blood-brain barrier breakdown, increasing susceptibility to nosocomial respiratory infections. We are designing a multifunctional therapy for PT-TBI to stop hemorrhaging, prevent infection, and reduce inflammation using a nanosilver platelet-like particle.
Necrosis is a form of lytic cell death that can occur in every multicellular organism, resulting in complex and poorly understood tissue outcomes, making understanding this phenomenon a significant challenge. Therefore, the overarching goal of my research is to understand the impact necrosis has on neighboring tissue.
One of the strongest genetic risk factors for Alzheimer’s disease (AD) is variations of the BIN1 gene. We are modeling BIN1 risk mutations using advanced genome editing approaches to generate isogenic human induced pluripotent stem cell (hiPSC) lines. This system will isolate the impact of each BIN1 variant and dissect cell type–specific mechanisms across neurons, astrocytes, and other glial cells.
I am interested in the relationship between dysregulated metabolism and neurodegeneration in the human brain. My research utilizes 3D organoids generated from human stem cells to disentangle pathways that distinguish healthy versus pathological states. The overall goal is to establish their mechanistic contribution to disease to uncover more effective therapeutic targets.
Non-invasively measuring the oxygen availability will deepen our understanding of tissue physiology, help evaluate implant engraftment and enable the development of theranostic treatments.
We utilize magnetic resonance (MR) oximetry through a sequence called proton imaging of siloxanes to map tissue oxygenation levels (PISTOL). Specifically, we aim to non-invasively assess oxygen levels in adipose tissue regions, optimize the design of regenerative scaffolds, and improve monitoring of engineered tissues after implantation.
Contact us
Program questions can be directed to Rebecca Gant at [email protected].